Spotlight Activity: The Social Cost of Climate Change Impacts on the Vulnerable
We are increasingly aware that climate change is creating health threats. Health Canada (HC) lists Canada’s most vulnerable populations as: children, seniors, the chronically ill, the low-income, the homeless, the disabled, outside workers, and those living off the land and in the North.
The Climate Atlas of Canada advises over 80% of Canadians live in urban areas and these numbers are growing. As of mid-2018, Canada’s population was 37 million of which ages 0-9 was 3,981,907 (11%), and ages 65 and older was 6,358,220 (17%). Few studies go beyond a general discussion of climate change vulnerability to investigate health equity implications. Extreme weather conditions such as rain, heat and cold worsen pre-existing conditions such as mental illness, respiratory and cardiovascular diseases, social isolation and drug and alcohol use. An established body of research shows health disparities lie in broader social and economic inequality and exclusion. The elderly and young are more susceptible to heat stress being less able to regulate their body temperature, sensitive to air pollution, and more vulnerable to weather events given mobility issues. Intrinsic factors such as age or disability, lower incomes, and use of certain medications can increase risks associated with extreme heat. Extrinsic factors such as inadequate housing, non-access to cooling centres or transportation can worsen risk factors.
Socio-economic impacts on community health and well-being of a changing climate involve increasingly extreme weather conditions, putting more demand on health care services (severe heat, air quality concerns, infectious diseases, aging populations, winter ice falls, malnutrition), disruption in social networks (power outages, wildfires, large scale disasters), interference with livelihoods (drought, crop failures), damages in housing and shelter (flood relocation, drownings) and infrastructure (food production and security, water management, energy production, storm sewers, drainage and sanitation systems, and health infrastructures). Special challenges for northern Canadians include dangerous travel, damaged infrastructure, threats to traditional food sources, loss of drinking water sources and related psychosocial and cultural heritage impacts.
The Lancet, a prestigious medical journal, in November 2018, identified 41 indicators to measure impact, adaptation, mitigation, economics, and the politics of climate change globally. It also worked collaboratively with the Canadian Medical Association, Canadian Public Health Association and Canadian Association of Physicians for the Environment (CAPE) producing a recent Canadian report confirming more people are being exposed to extreme heat in Canada (http://www.lancetcountdown.org/media/1418/2018-lancet-countdown-policy-brief-canada.pdf).
This report also states that Canada is not yet doing enough to reduce climate change emissions, estimating chronic exposure to PM2.5 air pollution results in 7,142 premature deaths every year and $53.5-billion in health-related costs per year. Recommendations included more coordination to track and monitor heat-related illness, improved communications to the public on heatwaves and worsening climate impacts, integrating climate change and health into the curriculum of all medical and health sciences facilities, increasing Canada’s adaptation targets, helping transition fossil fuel workers to greener jobs, enacting carbon pricing policies, and funding increased study into climate mental health impacts and psychosocial adaptation opportunities.
In recent years, greater efforts have been taken by public health and emergency management officials and non-profits to better prepare Canadians for climate change impacts on health. Canada’s Chief Public Health Officer’s 2014 report theme, a changing climate, discussed adaptive capacity in Canada as generally high but unevenly distributed between and within regions and populations. This important document is found at https://www.canada.ca/en/public-health/corporate/publications/chief-public-health-officer-reports-state-public-health-canada/chief-public-health-officer-report-on-state-public-health-canada-2014-public-health-future/public-health-in-a-changing-climate.html.
Another tool is the Air Quality Health Index, a health risk scale from 1-10 so you can adjust your activity levels. Visit https://weather.gc.ca/airquality/pages/index_e.html.
HC is developing a Health of Canadians in a Changing Climate: Advancing our Knowledge report, for 2021 release. Stakeholders are asking for in-depth information on climate change and health, vulnerable populations, and an inventory of health-adaptation best practices. Inquiries go to hc.ccha.secretariat.eccs.sc@canada.ca.
Most importantly, an expert panel released a game changer suite of indicators to measure progress on climate change adaptation and resilience including human health in June 2018. Indicators reflect priority areas identified in the Pan Canadian Framework on Clean Growth and Climate Change policy developed to achieve Canada’s commitment to the Paris Agreement. This is found at http://publications.gc.ca/collections/collection_2018/eccc/En4-329-2018-eng.pdf
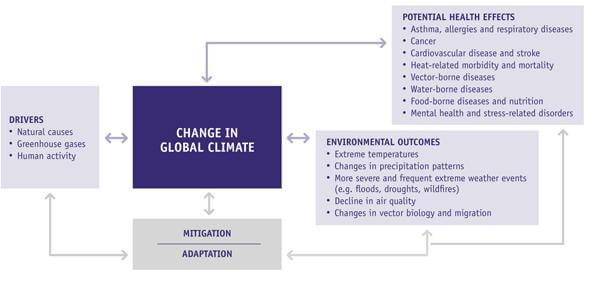
Figure: Pathways by which changes in climate can increase risks to health, adapted from Portier, C.J. et al. (2010), Chief Public Health Officer’s Report 2014.
Visit https://cape.ca/wp-content/uploads/2019/03/Press-Release-CC-Call-to-Action-Feb-5-updated-March-2019.pdf – a call to action from Canada’s Health Professionals February 5, 2019.
Status: Moving Forward
A widespread understanding of climate change as a central public health issue is vital through the health profession in delivering an accelerated response to health concerns. HC sees vulnerability assessments important to identify populations at risk, and implementation of adaptation options to reduce climate change effects. Several analytical frameworks exist to assess vulnerability and adaptive capacity and are widely used by public health. Adaptation strategies benefit from robust environmental health indicators of vulnerability and preparedness to prevent health impacts. Targeted research and reliable data is important to as a baseline to monitor adaptation measures and progress. Data and analysis gathered from public health surveillance systems and tools can support a number of further public health functions.
Thus the development of a low-carbon transition requires strong effort from Health Canada, and Climate Change and Environment Canada to work together in shaping our nation’s health for centuries to come. The recent Lancet and Expert Panel Canadian reports are showing the way.
Take Action
Adaptation tools and measures, such as heat alert and response systems, projections of vector-borne disease expansion and greening urban environments result in valuable co-benefits leading to improved human health and the environment. See Appendix. We ask for a closer alliance of Health Canada and Environment and Climate Change Canada to align health impact and climate change strategies together to ensure that Canada is 1.5°C compliant by 2030.
Send Action Alert Message to:
The Honourable, Ginette Petitpas Taylor, Minister of Health
Email: Ginette.PetitpasTaylor@parl.gc.ca
Mail: House of Commons, Ottawa, ON K1A 0A6
Phone: (613)992-8072
APPENDIX
- https://www.healthunit.com/climate-change – Assessment of vulnerability
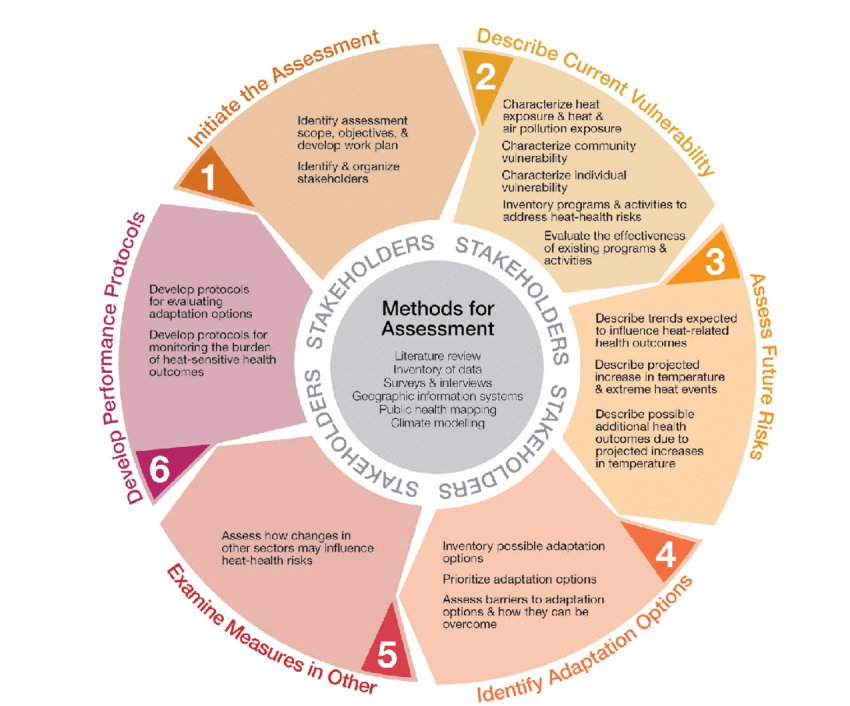
- Health Chapter – Canada in a Changing Climate: Sector Perspectives on Impacts and Adaptation – Scientific Figure on Research Gate. Available from: https://www.researchgate.net/figure/Steps-for-conducting-an-extreme-heat-and-health-vulnerability-assessment-Source-Health_fig8_264697905 [accessed 27 Jul, 2019]
FIGURE: Steps for conducting an extreme heat and health vulnerability assessment (Source: Health Canada, 2011a).


Leave a Reply
You must be logged in to post a comment.